
Question #1
A young mother brings her 6-month-old firstborn son for a health supervision visit. She states that the baby has been doing well and she has not noticed any abnormalities in his development, though her experience is really not very significant, she says. The boy is breastfeeding and is increasing the number of solid foods he eats with each passing day. He sleeps almost through the night and stopped having colic 2 months earlier. On physical examination the boy appears to be in no distress. He is in the 50th percentile for weight and length and his vital signs are normal. The health care provider performs a thorough neurologic exam in front of the mother, who is very curious about everything the health care provider is doing. On extension of the head, the boy flexes his arms and legs. When a finger is put in his palm, he flexes his hand, elbow and shoulder ipsilaterally. Tactile stimulation of the cheek prompts him to turn his mouth to that side, and touching the dorsum of his foot leads to a step-up movement. During a simulated fall, the baby reacts by extending his arms. The mother asks about each and every one of the newborn reflexes and when they are supposed to disappear. Which of the following is likely to be the one reflex that persists throughout life?
Answer:
The correct answer is C. Most reflexes are present at birth and disappear by age 4 to 6 months. The parachute reflex is described as extension of the infant's arms when a fall is stimulated. It appears at age 6 to 8 months and never disappears. The central nervous origin of this reflex is in the brain stem vestibular nuclei.
In Moro reflex, extension of the head leads to flexion of the arms and legs (choice A). It is present at birth and disappears at age 4 to 6 months. The central nervous origin of this reflex is in the brain stem vestibular nuclei.
In the grasp reflex, putting a finger in palm leads to flexion of the hand, elbow, and shoulder ipsilaterally (choice B). It is present at birth and disappears at age 4 to 6 months. The central nervous origin of this reflex is in the brain stem vestibular nuclei.
In the rooting reflex, stimulation of the cheek prompts turning of mouth to that side (choice D). It is present at birth and disappears at age 4 to 6 months. The central nervous origin of this reflex is in the brain stem vestibular nuclei.
In the placing reflex, stimulation of the dorsum of the foot leads to a step-up movement (choice E). It is present at birth and disappears at age 4 to 6 months. The central nervous origin of this reflex is also in the brain stem vestibular nuclei.
Reviewed on 2/28/13
The parachute reflex is a reflex that presents early in life (6-8 months) and never disappears. This reflex is the extension of the patient's arms when a fall is simulated. Patients may exhibit this reflex when rapidly falling asleep when they have the sensation that they are falling during the initiation of sleep
Question #2
A 40-year-old woman is brought to the emergency department following a suicide attempt with imipramine (Tofranil). Her fiancé found her unresponsive, with an empty bottle of the imipramine at her side. The imipramine had been his, and the prescription had been filled that morning. Her past medical history is significant for hypertension, atrial fibrillation, diabetes, and asthma. Her medications include furosemide, procainamide, glyburide, prednisone, and albuterol. She has no known drug allergies. She is afebrile, has a blood pressure of 100/60 mm Hg, pulse of 62/min, and respirations of 22/min. A gastric lavage yields multiple pill fragments. She is confused and somnolent, and has shallow respirations. Her physical examination is otherwise unremarkable. On an electrocardiogram, which of the following abnormalities would most likely reflect possible cardiac toxicity?
Answer:
The correct answer is B. A prolongation of the QT interval is highly predictive of both cardiac and CNS toxicities from tricyclic antidepressant ingestion. This medication has high lethality associated with its overdose because of its cardiac effects.
Left deviation of the QRS axis (choice A), which can be seen with conditions such as left ventricular hypertrophy, left bundle branch block, and left posterior hemiblock, is not typically associated with tricyclic cardiac toxicity.
Pre-excitation syndromes (choice C) are not seen with tricyclic toxicity, but they can be seen Wolff-Parkinson-White syndrome and Lown-Ganong-Levine syndromes, which are caused by the congenital presence of accessory pathways that lead to the ventricles becoming pre-excited. These conditions are not associated with the use of tricyclic antidepressants.
Neither ST-segment depression (choice D) nor T-wave inversion (choice E) is directly associated with cardiac toxicity from tricyclic overdose. These changes may be seen, however, in conjunction with the more classic ECG manifestations of tricyclic toxicity (prolonged QT interval, right axis deviation) if the resulting cardiac toxicity leads to diminished coronary perfusion and ischemia.
Reviewed on 4/17/14
QT prolongation may be secondary to the use of various medications or from electrolyte abnormalities or it may be an inherited condition (prolonged QT syndrome). Tricyclic antidepressants, certain antiarrhythmics (especially class III Vaughn Williams antiarrhythmics such as amiodarone), and hypocalcemia, hypomagnesemia, and hypokalemia may lead to prolonged QT syndrome. Patients who have this condition have an increased risk for syncope, ventricular arrhythmias (especially torsades des pointes), and sudden cardiac death.
Question #3
A patient with systemic lupus erythematosus (SLE) very much wants to become pregnant. What should her health care provider tell her regarding pregnancy?
Answer:
The correct answer is E. Systemic lupus erythematosus (SLE) predominantly affects younger women, and so the question of lupus and pregnancy may arise frequently in clinical practice. Patients who have SLE have an increased incidence of spontaneous abortion, fetal death in utero, and prematurity. The mother may experience an exacerbation in the activity of her disease in the third trimester or peripartum period, and it may be difficult to distinguish between active SLE and preeclampsia. Therapy of pregnant patients who have SLE is problematic, and these women should have their prenatal care provided by a specialist.
Congenital malformations (choices B, C, and D) are not a complication of pregnancy in SLE patients.
Reviewed 8/24/14
Patients who have SLE may develop antiphospholipid antibodies, which is associated with high rates of fetal loss. Even without the presence of antiphospholipid antibodies, women who have SLE have a higher rate of fetal loss than patients who do not have SLE.
Question #4
A 54-year-old woman comes to the emergency department with severe left-sided flank pain that is referred to the left labia majora. She is very uncomfortable lying still on the stretcher and is continuously shifting, trying to find a comfortable position. A nonenhanced helical CT scan shows a 10-mm ureteral stone at the ureteropelvic junction. She has a normal coagulation profile. Which of the following would most likely be the best therapy in this case?
Answer:
The correct answer is B. Extracorporeal shock wave lithotripsy (ESWL) is the most commonly used method to fragment urinary stones and allow their passage. Pregnancy and coagulation problems are contraindications. The first one is ruled out by her age; the second one we have been told she does not have. Because the stone is 10 mm, it is less likely to pass on its own because of its large size.
Waiting for spontaneous passage (choice A) would have been perfect for a much smaller stone (3 mm) that had already negotiated most of the ureter. A 7-mm stone way up at the ureteropelvic junction has a very small chance of spontaneous passage.
Retrograde endoscopic approaches (choices C and D) are more invasive than ESWL. They would not be the first choice for this scenario.
Open surgical removal (choice E) would have been good for a much bigger stone. A huge target (3 cm or larger) could indeed be fragmented by ESWL, but then we would be contending with dozens of still very large stones. In those cases, a direct approach to extract the huge intact stone would work better.
Reviewed on 5/3/14
Most calculi >10 mm will not pass spontaneously. Current surgical management options include cystoscopic placement of ureteral stents, nephrostomy with urine drainage, extracorporeal shock wave lithotripsy, and ureteroscopy with stone fragmentation (usually with laser lithotripsy).
Question #5
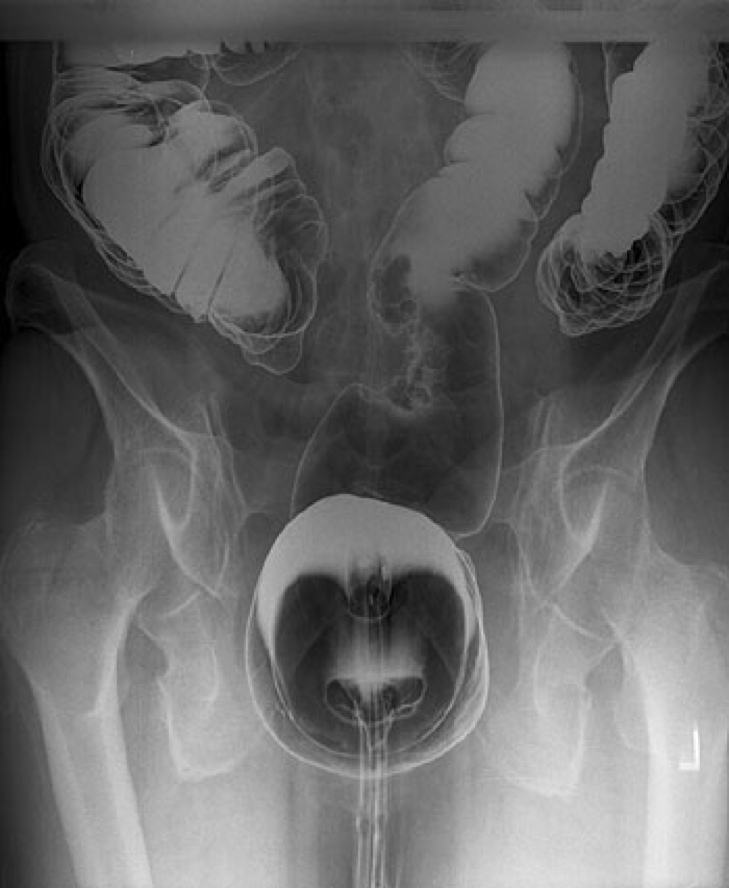
A 69-year-old woman comes to the health care provider for a periodic health maintenance examination. She has no complaints. She takes 1,500 mg of calcium daily, a multivitamin, and daily aspirin. She exercises regularly, eats a fairly healthy diet, and does not smoke cigarettes. She drinks a couple of glasses of wine with dinner each evening and smokes marijuana occasionally with a friend who has glaucoma. She is concerned about her risks for breast, ovarian, and colon cancer because she has friends with each of these diseases. Breast and pelvic examination are unremarkable. A mammogram is normal. Findings from a barium enema are shown. Which of the following is the most common presenting symptom of this condition?
Answer:
The correct answer is C. The barium enema demonstrates an irregular lesion that causes obstruction in the sigmoid colon. This finding on barium enema is highly suspicious for adenocarcinoma. Cancers arising in the left and sigmoid colon are characterized by rectal bleeding, obstructive symptoms, and constipation possibly alternating with diarrhea. Stools may develop a narrow caliber as the tumor encroaches onto the lumen.
Although anemia (choice A), Blumer shelf (metastasis to the pelvic cul-de-sac) (choice B), Virchow node (palpable lymph node in the left supraclavicular space) (choice D), and weight loss (choice E) can be associated with cancers of the left and sigmoid colon, they are more commonly associated with highly advanced colon cancer.
Reviewed on 11/13/14
Remember the most common signs for colon masses; some of them will depend on the location of the mass.
Question #6
A 49-year-old man is recuperating in a hospital after having sustained a recent cerebrovascular accident that damaged part of his right temporal lobe. His wife and children are at his bedside day and night. They want to actively participate in his rehabilitation but specifically ask the health care provider what they can expect from him in the future. Once the patient has recuperated from the immediate effects of his stroke, to which of the following psychiatric disorders will he be most predisposed?
Answer:
The correct answer is C. Any event that affects the vasculature, such as a myocardial infarction or a cerebrovascular accident (CVA), has been shown to increase the risk of major depressive disorder in the months that follow. The pathophysiology of such a development is unclear, but is thought to be related to the effects of serotonin on vascular physiology.
Conversion disorder (choice A) is a disorder of physiological complaints that are related to social stressors; it has not shown to be related to vascular events.
Narcolepsy (choice B) is a sleep disorder characterized by irresistible attacks of refreshing sleep.
Schizophrenia (choice D) is a thought disorder characterized by disturbances in language, thought content, and perception.
Substance abuse (choice E) is not increased in incidence in individuals after a CVA.
Reviewed on 2/28/13
Patients who suffer a stroke have a high probability for developing major depression disorder. The etiology for this depression is probably multifactorial, with the stroke itself affecting the brain plus the patient's physical impairment adding to the patient's psychologic impairment
Question #7
A patient who is being treated for hypertension related to a myocardial infarction that occurred 2 hours ago is medicated with IV nitroprusside (Nipride). Which of the following is the expected action of this drug?
Answer:
The correct answer is E. Nitroprusside is a very useful IV agent that causes dilatation of both arterioles and venules. It has a very rapid onset of action and is typically used in an emergency department or intensive care unit situation. It can be titrated to effect on a drip-to-drip basis. It is used in settings in which the blood pressure needs to be carefully controlled. It is listed on ACLS protocols as one of the treatments (along with the combined alpha- and beta-blocker labetolol) for hypertensive emergency/hypertensive urgency. Nitroprusside can improve perfusion of vital organs and reduce the workload of the heart because it is both an arteriolar and venodilator. Problems sometimes encountered with this drug include hypotension (best avoided by starting with a low dose and continuously monitoring systemic arterial and pulmonary capillary wedge pressures) and accumulation of toxic metabolite (thiocyanate) of cyanide in patients who have liver or renal failure. Many physicians prefer to use IV nitrate rather than nitroprusside because of its lesser toxicity.
Reviewed on 4/17/14
Sodium nitroprusside and labetolol are parenteral agents indicated for treating hypertensive urgency and hypertensive emergency. They may also be used to treat hypertension that is related to sympathomimetic drug use (such as cocaine, amphetamines, phenylpropanolamine, MAO-related hypertensive crisis). As a potent arterial and venous dilator, it is able to reduce both preload and afterload. Nitroprusside is typically administered with a beta-blocker, because its potent nitroprusside-induced vasodilation induces a strong compensatory tachycardia that might increase stress to the system.
Question #8
A 63-year-old woman comes to the emergency department with severe abdominal pain. She reports the pain is epigastric and worse with eating. There is some radiation to the back. There is associated diarrhea that is described as "fatty." Symptoms have been present for 3 to 4 months. Her medical history is significant for 2 episodes of acute pancreatitis, hypertension, and hyperlipidemia, but she takes no medications for these disorders. Her temperature is 38.3ºC (100.9ºF), blood pressure 160/90 mm Hg, pulse 143/min, and respirations 16/min. Physical examination shows epigastric tenderness, mild distention, and decreased bowel sounds. She appears uncomfortable and in moderate distress. An obstruction series reveals only scattered pancreatic calcifications. Laboratory studies show:
| Amylase | 45 U/L (normal 23-140 U/L) |
| Lipase | 10 U/L (normal <160 U/L) |
| Albumin | 2.8 g/dL (normal 3.4-5.4 g/dL) |
| AST | 98 IU/L (normal <40 IU/L) |
| ALT | 45 IU/L (normal <40 IU/L) |
| Total bilirubin | 1.1 mg/dL (normal <1.9 mg/dL) |
Which of the following is the most likely underlying etiology for this patient's symptoms?
Answer:
The correct answer is A. This patient has chronic pancreatitis. The finding of calcifications in the pancreas is a good clue to this patient's diagnosis. Amylase and lipase can be normal or elevated, depending on how much intact pancreas is left. Seventy percent of chronic pancreatitis is caused by alcohol ingestion. Our patient's malnutrition, as evidenced by her low albumin and her AST to ALT ratio of 2:1, is consistent with alcoholic hepatitis. The treatment is pain relief, a low-fat diet with medium chain triglycerides, vitamins, and pancreatic enzyme replacement. The remaining 30% of chronic pancreatitis is idiopathic (choice E).
Elevated triglycerides (choice B) are a rare cause of acute pancreatitis, not chronic pancreatitis. Triglyceride levels in these patients are usually >1,000 mg/dL.
Gallstones (choice C) are an important cause of acute pancreatitis but are not typically associated with chronic disease. Patients who have gallstone pancreatitis are usually overweight, fertile, and in their forties. Correction is by ERCP removal or laparoscopic cholecystectomy with common duct exploration and removal of the choledocholithiasis.
Hypercalcemia (choice D) is a rare cause of acute pancreatitis. Pancreatic calcifications seen on obstruction series do not represent elevated serum calcium levels. Hypocalcemia can complicate acute pancreatitis as a result of saponification of fats, which takes place due to pancreatic insufficiency because of acute pancreatitis.
Reviewed on 5/4/14
Chronic pancreatitis is most often diagnosed when calcifications of the pancreas are noted on abdominal CT scan. The most common cause of chronic pancreatitis in the United States is alcoholism. AST to ALT ratio of at least 2:1 is consistent with alcoholic hepatitis. Other causes of chronic pancreatitis include untreated gallstone disease, medications, celiac disease, and family history.
Question #9
A 20-year-old woman comes to the health care provider because of left lower quadrant pain for 2 months. She states that she first noticed the pain 2 months ago but now it seems to be getting worse. She has had no changes in bowel or bladder function. She has no fever or chills and no nausea, vomiting, or diarrhea. The pain is intermittent and sometimes feels like a dull pressure. Pelvic examination is significant for a left adnexal mass that is mildly tender. Urine hCG is negative. Pelvic ultrasound shows a 7-cm complex left adnexal mass with features consistent with a benign cystic teratoma. Which of the following is the most appropriate next step in management?
Answer:
The correct answer is E. This patient has a presentation and findings that are most consistent with a benign cystic teratoma (dermoid). Dermoids are a type of ovarian germ cell tumor. Germ cell tumors are the most common type of ovarian neoplasm in females under the age of 20 years, and dermoids are the most common benign ovarian neoplasm. Dermoids can range in size from small masses that are noted incidentally on ultrasound and cause no symptoms, to large cysts that cause pain and pressure, as this patient has. Laparotomy is the most appropriate next step in the management of this patient because as adnexal masses enlarge (especially when they become greater than 5 cm) the risk for ovarian torsion increases. Laparotomy with removal of the dermoid therefore is indicated to prevent torsion. Also, this patient's mass is causing her symptoms of pain and pressure, and on that basis should be removed. Finally, although the mass most likely is a dermoid, this is not certain without pathologic diagnosis, and therefore the cyst should be removed and evaluated by a pathologist. At the time of surgery, close examination should be made of the other ovary, because dermoids may be found bilaterally in more than 10% of cases.
To repeat pelvic examination in 1 year (choice A) would not be correct management. This patient is symptomatic with a 6-cm ovarian mass that is at risk for torsion. She therefore should be managed surgically.
To repeat pelvic ultrasound in 6 weeks (choice B) is appropriate for some adnexal masses. For example, in a young woman who has a small complex cyst that appears consistent with a corpus luteum, it may be most prudent to recheck an ultrasound in 6 weeks to see if the cyst has resolved. This patient, however, is symptomatic with a 6-cm cyst that appears to be a dermoid, which will not resolve spontaneously. She therefore requires surgery.
To prescribe the oral contraceptive pill (choice C) may help to prevent future ovarian cysts, but it will not resolve this cyst, which requires surgical management.
To perform hysteroscopy (choice D) would not be indicated. Hysteroscopy is used to evaluate the uterine cavity and fallopian tubes and would not be used for management of an adnexal mass.
Reviewed on 8/28/14
Laparotomy is indicated in a patient who has an adnexal mass when:
Question #10
A 30-year-old woman with a history of tonic-clonic seizures complains of double vision, thickened gums, and growth of facial hair since starting a new medication. Which of the following anticonvulsant medications is most likely responsible for her symptoms?
Answer:
The correct answer is D. Diplopia, gingival hyperplasia, and hirsutism are classic side effects of phenytoin. Other side effects include nystagmus, sedation, ataxia, and enzyme induction. Phenytoin is used in the treatment of grand mal and tonic-clonic seizures. It is not used for absence seizures.
Carbamazepine (choice A) does produce diplopia, but not the other symptoms in this vignette. It can also produce ataxia, enzyme induction, and blood dyscrasias. It is useful in tonic-clonic and partial seizures and in tic douloureux.
Ethosuximide (choice B) causes GI distress, headache, and lethargy. It is used exclusively for absence seizures.
Phenobarbital (choice C) is used for grand mal and partial seizures. It causes sedation, enzyme induction, and dependence.
Valproic acid (choice E) causes GI distress, hepatotoxicity, and inhibition of drug metabolism. It can be used for all seizure types but is particularly useful in myoclonic and petit mal seizures.
Reviewed on 7/3/14
Phenytoin (Dilantin) use is associated with several well-known side effects such as gingival hyperplasia, hepatotoxicity, thrombocytopenia, leukopenia, agranulocytosis, and megaloblastic anemia when taken orally. Phenytoin results in severe cardiac adverse events when given intravenously, which can include ventricular fibrillation and cardiac conduction abnormalities.
Looking for more practice? Practice with test-like questions and get comprehensive explanations.
Learn more about Kaplan’s Physician Assistant boards prep: Live Online classes, Live Review, and Qbank.
Fill out the information below to get the answers and explanations. We’ll also email you free tips, admissions advice, exclusive offers, and other content aimed specifically to help you do better on Test Day.